Influenza Vaccine Technologies: What's New to Fight the Flu
Deadly Fungus Spreading Like Wildfire Can Cause Nasty Infection - Symptoms To Look For
Candida auris has been spreading rapidly throughout the US, and the rest of the world, with potentially deadly consequences due to its difficulty to diagnose and resistance to many antifungal treatments
There is growing concern about the rapid spread of the potentially deadly fungal infection(Getty Images/iStockphoto)
Fears are growing over a dangerous and deadly fungus which is spreading at an alarming rate, particularly in healthcare settings, and is proving resistant to traditional treatments.
Back in 2016, hospitals in New York State identified a rare and potentially lethal final infection never before seen in the US. Researchers found it had been present in the country since at least 2013, with the infection first found in humans only four years prior, in 2009.
Candida auris can cause severe illness and has an estimated mortality rate of anywhere between 30 and 60 per cent, with particular risk in healthcare settings or for people with underlying serious medical problems. Due to the severity, rapid spread, and resistance to treatment, it's been marked as a globally emerging public health threat.
The Centers for Disease Control and Prevention (CDC) has said it is concerned about the fungus for three main reasons. First, it is "often multidrug-resistant" with some strains resistant to all three available classes of antifungals.
Second, it is "difficult to identify with stand laboratory methods" and can be easily misidentified, which could lead to inappropriate treatment or management. And thirdly, it has caused outbreaks in healthcare settings, which can spread rapidly.
'Last of Us' fungus with 60 percent mortality rate is new 'global health threat'
The potentially invasive fungal infection can affect multiple parts of the body (AP)
When Candida auris was first spotted spreading, CDC medical epidemiologist for the mycotic disease branch Meghan Marie Lyman said cases were linked to people who had travelled to the US from other locations. Now, she said, most cases are acquired locally.
IIn the US there were 2,377 confirmed clinical cases diagnosed last year, 2022. That represents an increase of more than 1,200 per cent since 2017. In Europe, a survey last year found cases nearly doubled from 2020 to 2021.
In March, a CDC press release noted the seriousness of the issue. Public health agencies are focused primarily on strategies to mitigate transmission in healthcare settings and protect the most vulnerable. Ms Lymann said: "it's kind of an active fire they're trying to put out."
Candida auris is a fungal infection which is part of the yeast family(Getty Images/Science Photo Library RF)
The sudden explosion of the fungal infection, which was first found in humans less than 15 years ago, has been linked to climate change in one prominent theory. While humans and mammals have warmer body temperatures than most fungal pathogens can handle, rising temperatures could allow fungi to develop tolerance to warmer environments.
This means that while we were previously protected from infections by our warm body temperatures, we may lose resistance as fungi become more acclimatised to warmer temperatures. Some researchers think this is what's happening with Candida auris.
With no prior record of infection in humans, the final disease spontaneously emerged 14 years ago on three continents; Venezuela, India and South Africa. One thing that stood out to experts was the locations - the climates in all three places are quite different.
Candida auris can be difficult to diagnose, not only due to its rarity, but because common symptoms can be linked to many other causes. So which symptoms should you be looking out for? We've broken down all you need to know about the terrifying, and potentially deadly, infection below.
Candida auris symptomsThe most common symptoms of Candida auris include fever, low blood pressure, and sepsis. These can all have many causes, especially in patients who are in a healthcare setting and have spent considerable time there, who are most at risk.
Candida auris was first reported in Japan in 2009, with the species isolated from the external ear canal of an inpatient in a Japanese hospital. The fungal infection has caused infections of the bloodstream, wound and ears.
It has also been isolated from respiratory and urine samples, according to the CDC, though it's unclear if it can cause infections in the lung or bladder.
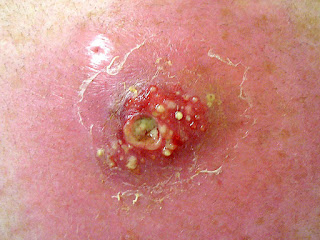
Candida auris can cause infections of wounds(Getty Images)
Symptoms of Candida auris may not be noticeable, as patients are often already sick in hospital with another serious illness or condition. It also depends on the part of the body affected.
Testing for the potentially lethal fungal infection is not easy, either. Often, it's misidentified as other types of fungi unless specialised laboratory technology is used.
Show more
In tests, blood is placed in a nutrient-rich medium to allow any infectious organism to grow and become more detectable. Dr Luis Ostrosky, a professor of infectious diseases at McGovern Medical SChool at UTHealth Houston, said that this misses around half of cases.
"Our gold standard is a little bit better than flipping a coin," he explained. He added there is a newer technology that improves bloodstream detection but it's expensive and not widely available in hospitals.
How serious is Candida auris?Candida auris is described as a potentially invasive infection, with its ability to get to different parts of the body - including the blood, brain, and other parts of the body. Its invasive nature means it can have serious, and even fatal, consequences.
While most Candida is treatable, one of the most worrying aspects of Candida auris is its resistance to treatment. There are three main classes of antifungals widely used - azoles, polyenes and echinocandins.
Show more
More than 90 per cent of Candida auris strains detected are resistant to azole treatments, with several studies finding high percentages resistant to polyene and even echinocandin resistance reportedly emerging in some countries.
Combined with the fact that the most at risk are those with underlying conditions, or who spend significant time in healthcare settings - it can be a deadly combination. Those most at risk of the often resistant infection are, in fact, those who are most vulnerable health-wise to begin with.
People who have recently spent time in nursing homes, or who have lines and tubes going into their body (such as breathing tubes, feeding tubes, and central venous catheters) seem to be at most risk, according to the CDC. There are also other risk factors which are similar for other types of Candida infections - recent surgery, diabetes, recent courses of antibiotics and antifungals.
Mystery Outbreak Of A Deadly, Paralyzing Disease Has Experts Baffled
A national state of emergency has been declared in Peru as doctors battle an outbreak of a rare disease that can cause lifelong paralysis or death.
More than 230 cases of Guillain-Barré syndrome have been reported in the South American country, with more than half the cases occurring in a brief five-week period from June to July.
Normally a rare disorder, GBS typically strikes only about 3,000 people per year in the US, according to Johns Hopkins Medicine.
Four people in Peru have reportedly died of the disease since the beginning of the year, and the still-unknown cause of the outbreak has health officials scrambling.
"I think the origins of this [outbreak] remain still not completely investigated," Dr. William Schaffner, an infectious disease specialist at Vanderbilt University Medical Center in Nashville, Tennessee, told Healthline.
"We haven't solved that puzzle," Schaffner added.
Peru, with numerous tourist attractions including archaeological sites like Machu Picchu, remains popular with travelers, though officials are warning that common-sense precautions are in order.
What is Guillain-Barré syndrome?When Guillain-Barré syndrome occurs, it typically follows an upper respiratory or gastrointestinal infection, such as the flu, COVID-19 or gastroenteritis. In some cases, it's seen after a surgical procedure, an injury or a reaction to an immunization, including the COVID-19 vaccine.
GBS is a neurological disorder in which the immune system attacks the nervous system. The first symptom is often a tingling, "pins-and-needles" sensation in the legs, which can gradually creep upward to the arms and upper body.
This feeling can strike quickly or may develop slowly over several weeks. Other symptoms include difficulty breathing, double vision, unsteady walking, fever and problems with bladder control or bowel function.
In severe cases, muscles may not function at all, resulting in paralysis, and even breathing becomes difficult, making GBS a medical emergency that needs to be treated promptly.
There is no cure for GBS, and even among those people who recover, there is often some lingering paralysis or nerve damage. Recovery can take from six months up to several years.
The World Health Organization issued a statement on Tuesday about the outbreak, noting that a similar outbreak of GBS with about 700 cases occurred in 2019 in Peru.
Health officials determined that the 2019 outbreak was largely due to infections caused by the Campylobacter jejuni bacteria, which is a common precursor of GBS.
Campylobacter infection is the leading cause of diarrheal illness in the US, according to the Centers for Disease Control and Prevention. It's usually caused by eating foods or drinking water that are contaminated with bacteria.
"It takes very few Campylobacter bacteria to make someone sick," the CDC states. "A single drop of juice from raw chicken can contain enough bacteria to infect someone."
And Campylobacter infection is the most commonly identified cause of Guillain-Barré syndrome. Indeed, laboratory testing in the current outbreak in Peru found Campylobacter infection in many of the GBS cases, according to the WHO.
More cases of Campylobacter infection occur in summer than in winter. Health experts advise caution, focusing on hand hygiene and food choices — especially for people traveling to areas with GBS caused by bacterial infections.
But safe food and water precautions are important for people everywhere: In 2015, testing by the National Antimicrobial Resistance Monitoring System found Campylobacter on 24% of raw chicken bought from retailers in the US.
When it comes to food safety, there are simple, common-sense strategies you can use to reduce your risk of infection with Campylobacter and other germs, Schaffner said.
"As one of my past professors used to say — he was an expert in travel medicine — don't eat anything that you can't either cook or peel," Schaffner added.
France Travel Warning Over Outbreak Of Deadly Infection - 6 Ways To Protect Yourself
French health officials say the country has seen a surge in the number of people being admitted to hospital with tick-borne encephalitis, with cases appeared to be particularly high in the Auvergne-Rhône Alpes region
The Auvergne-Rhône Alpes region is now an important area of TBE circulation (Image: Getty Images)
Brits travelling to one of France top tourist destinations have been warned over a potentially lethal disease outbreak.
The country has seen a huge surge in cases of tick-borne encephalitis in recent months, with the hospitalisation rate now at 94%., according to public health chiefs. The cases appear to be concentrated around a region in the French Alps.
Some 61 cases of the disease were diagnosed as having been caught in France, and those travelling there for summer holidays have been warned to watch out for the bugs which can be carriers.
Tick-borne encephalitis (TBE) is a rare but potentially fatal disease affecting the brain and central nervous system. Encephalitis, which is the medical term for inflammation of the brain, can be caused by disease carried by ticks, a common bug known to latch onto humans and animals.
It can be transmitted to humans by bites often during leisure activities, in humid wooded areas such as camping, hiking, and mushroom picking - all popular activities in the ski resort region which is also regularly visited during the summer months.
In 40% of cases, it can lead to long-lasting neurological problems. TBE has an incubation period of one to two weeks, meaning it can take up to 14 days between catching the disease before symptoms appear. Signs of TBE include flu-like symptoms such as fever, headache and chills.
The Auvergne-Rhône Alpes region is now an important area of TBE circulation, authorities have confirmed, with Haute-Savoie department reporting the highest number of cases in this two year period. Cases are now being reported in Ardèche department.
More than a third (37%) of cases in the two years up to May of this year resulted in potentially-fatal meningitis, France's health body said, while 38% also resulted in encephalitis, 13 per cent got meningoencephalitis, and three per cent encephalomyelitis. Ten per cent of patients had no neurological signs.
Ninety-four percent of cases required admission to hospital, although thankfully there were no deaths. Public Health France has now warned tourists should protect themselves from tick bites while outdoors.
Parents of young children in particular have been urged to carefully inspect their children after walking in rural areas or woodlands in endemic regions of up to 1,500 meters altitude, between spring and autumn. As well as bites it can also be transmitted via contamination through consuming raw dairy products. The main way to protect yourself it to wear protective clothing against tick bites.
How to protect yourself from tick bitesSmall in size, ticks are difficult to spot. When walking in the forest, in meadows or when gardening, a few tips to follow can protect you from bites:
Encephalitis usually starts off with flu-like symptoms, such as a high temperature and headache. More serious symptoms come on over hours, days or weeks, including:
Dial 999 for an ambulance immediately if you or someone else has these serious symptoms.

Comments
Post a Comment